This web page was produced as an assignment for Genetics 564, an undergraduate capstone course at UW-Madison
What is Ovarian Cancer? [1,2]
|
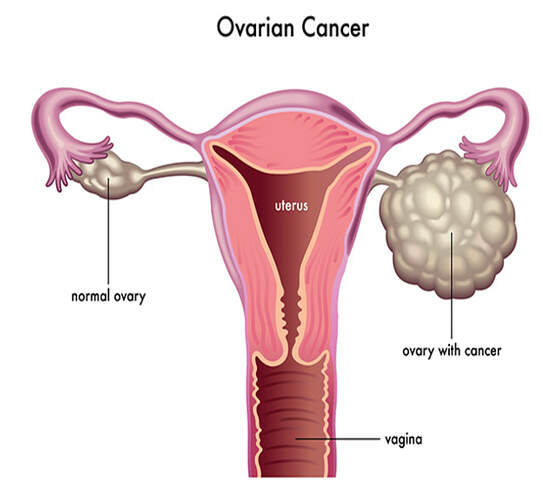
Although cancer can come originate from a multitude of different tissues and various causes, every cancer shares a central feature –they are the result of uncontrolled cell growth. Although ovarian cancer is not a common cancer, it does account for the most deaths of any gynecological cancer [1]. Ovarian cancer begins when tumors form from one of three ovarian cell types [2]:
|
What is Mestastasis [3]
Cancer becomes particularly dangerous when it spreads to other tissues in a process known as metastasis [3]. Using either the lymph vessels or the blood, a metastatic tumor can invade another part of the body [3]. The video linked below provides an excellent explanation of how cancers spread to other tissues, and why this is dangerous for human health [3].
However, it is important to understand that not all tumors are cancerous. Some ovarian tumors, including epithelial ones, may be benign (non-cancerous), or borderline. These borderline tumors may spread outside the ovary, but cannot invade supporting tissues [2].
Signs and Symptoms of Ovarian Cancer
|
Symptoms of Ovarian Cancer [1,2,3,4]:
|
Inspirational author, and performer, Jenny Allen, shares some of the symptoms and experience being diagnosed with ovarian cancer.
|
These symptoms are not a diagnoses of ovarian cancer and may be the result of other serious diseases. If you are experiencing any of the above symptoms contact your doctor immediately.
Risk Factors for Ovarian Cancers [3]
- A family history of ovarian cancer or Lynch syndrome (see Genetic Risk Factors below)
- Obesity.
- Tall height.
- Endometriosis
- Postmenopausal hormone therapy.
Genetic Risk Factors [5]
A patient’s genetic background plays an important role in determining their risk for developing ovarian cancer. Harmful mutations in either the BRCA1 or BRCA2 have been found in 90% of families with both ovarian and breast cancer and accounts for 50% of families with breast cancer [5]. BRCA1 and BRCA2 function as tumor suppressors and encode proteins that function in an important DNA repair pathway known as Homologous Recombinational Repair (HRR). Through HRR, cells can accurately and safely repair a specific form of damage in DNA known as a double-strand break (DSB). Mutations that prevent either of the BRCA proteins from properly functioning prevents DSB’s from being repaired in an accurate manner, leading to additional mutations occurring in the cell’s DNA and increases the risk of developing breast/ovarian cancer [5].
Although BRCA1 and BRCA2 mutations are found in numerous ovarian cancer patients, there are other genetic risk factors including mutations in RAD51C, RAD51D, and STK11, all of which are included in multi-gene testing [5]. If you or a family member have received positive test results for any of the above genes, please discuss these results your health care professional.
Although BRCA1 and BRCA2 mutations are found in numerous ovarian cancer patients, there are other genetic risk factors including mutations in RAD51C, RAD51D, and STK11, all of which are included in multi-gene testing [5]. If you or a family member have received positive test results for any of the above genes, please discuss these results your health care professional.
RAD51D and Ovarian Cancer [6,7]
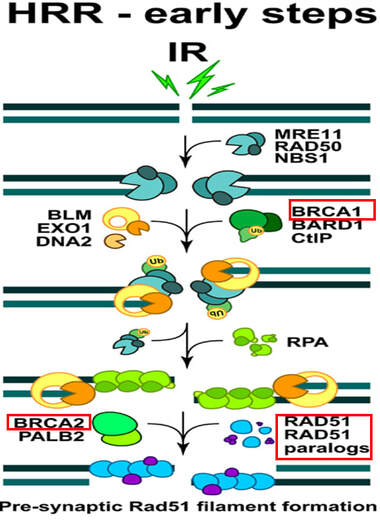
The RAD51D gene encodes a protein that plays an essential role in the Homologous Recombination Repair (HRR) pathway that repairs double-strand breaks in damaged DNA. In order to interact with a template for accurate DNA repair, RAD51D participates in forming the BCDX2 complex that recruits RAD51 proteins to form a filament that is essential for the early stages of HRR. However, there is evidence that RAD51D may function in other steps of the HRR pathway, as well as maintaining telomeres [6].
Some types of mutations in RAD51D gene eliminates or alters its function in the HRR pathway. Because of this, error-prone repair processes are recruited, resulting in additional mutations that accumulate in the DNA. As these ovarian cells amass more mutations, an individual’s risk for developing ovarian cancer increases [7].
Women who have tested positive for a pathogenic RAD51D mutation have a 10-12% chance of developing ovarian cancer which is approximately 5-6 times greater than the average woman [7]. Estimates for the frequency of RAD51D mutations ranges from 0.35 – 1.1% [8]; however more research will need to be conducted to better estimate the frequency of these mutations, as well as differences across multiple populations. [9].
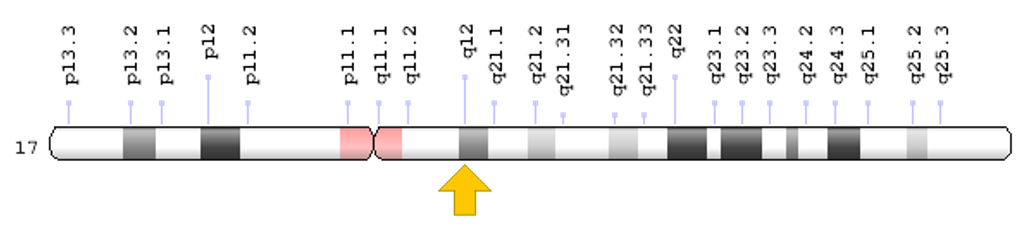
The RAD51D gene is located on chromosome 17 at position q12, as indicated by the yellow arrow.
What Treatments are Available? [10]
Treatment for ovarian cancer varies from patient to patient, and should be discussed with your physician. Typical treatments include a combination of surgery and chemotherapy.
Surgery [10]:
If cancer is present in only one ovary, surgery may be recommended to remove the affected ovary, while leaving the other intact. However, if both ovaries are cancerous, removal of both ovaries may be an option. Finally, if the cancer has extended beyond the ovaries, your physician may recommend the removal of the ovaries, uterus and both Fallopian tubes.
Chemotherapy [10]:
Chemotherapy is a type of drug treatment that targets cells that are quickly growing. While chemotherapy is able to target cancer cells, the drug treatment can also target healthy cells, leading to some unpleasant side effects. Chemotherapy drugs are typically injected into a vein or administered orally. Chemotherapy may be used in conjunction with surgery, being administered before or after a surgical procedure to optimize the number of cancer cells targeted by the treatment.
Targeted therapy [10]:
Targeted therapy takes advantage of impressive medications that exploit weaknesses in cancer cells. If ovarian cancer returns after prior treatment, or a patient's cancer is resistant to other treatments, targeted therapy may be recommended.
Surgery [10]:
If cancer is present in only one ovary, surgery may be recommended to remove the affected ovary, while leaving the other intact. However, if both ovaries are cancerous, removal of both ovaries may be an option. Finally, if the cancer has extended beyond the ovaries, your physician may recommend the removal of the ovaries, uterus and both Fallopian tubes.
Chemotherapy [10]:
Chemotherapy is a type of drug treatment that targets cells that are quickly growing. While chemotherapy is able to target cancer cells, the drug treatment can also target healthy cells, leading to some unpleasant side effects. Chemotherapy drugs are typically injected into a vein or administered orally. Chemotherapy may be used in conjunction with surgery, being administered before or after a surgical procedure to optimize the number of cancer cells targeted by the treatment.
Targeted therapy [10]:
Targeted therapy takes advantage of impressive medications that exploit weaknesses in cancer cells. If ovarian cancer returns after prior treatment, or a patient's cancer is resistant to other treatments, targeted therapy may be recommended.
Gap in Knowledge
Previous research has shown that loss of function mutations in RAD51D contribute to large deletions in ovarian hamster cells, suggesting that RAD51D may play a protective role against large-scale deletions [11]. However, the mechanism by which RAD51D prevents these large deletions remains unknown. Surprisingly, RAD51D's role in other cancers remains unknown with recent meta-analyses establishing RAD51D as an ovarian exclusive, high risk allele [12,13]. Yet, it is unknown why RAD51D favors ovarian cancer in a tissue-specific manner.
References: |
- MedlinePlus. Ovarian Cancer (2019, Jan. 25). Retrieved from https://medlineplus.gov/ovariancancer.html
- American Cancer Society. What is Ovarian Cancer? (2018, April 11). Retrieved from https://www.cancer.org/cancer/ovarian-cancer/about/what-is-ovarian-cancer.html
- National Cancer Institute. Ovarian Epithelial, Fallopian Tube, and Primary Peritoneal Cancer Symptoms, Tests, Prognosis, and Stages (PDQ®)–Patient Version (2019, January 23). Retrieved from https://www.cancer.gov/types/ovarian/patient/about-ovarian-cancer-pdq
- Centers for Disease Control and Prevention. What are the Symptoms of Ovarian Cancer? (2017, February 9). Retrieved from https://www.cdc.gov/cancer/ovarian/basic_info/symptoms.htm
- National Cancer Institute. BRCA Mutations: Cancer Risk and Genetic Testing (2018, Jan 30). Retrieved from https://www.cancer.gov/about-cancer/causes-prevention/genetics/brca-fact-sheet
- Gene Cards. RAD51D Gene. Retrieved 2/3/2019 https://www.genecards.org/cgi-bin/carddisp.pl?gene=RAD51D
- Ambry Genetics. Understanding Your Positive RAD51D Genetic Test Result. Retrieved 2/3/2019 https://www.ambrygen.com/sites/default/files/web/understanding_your_results/cancer/rad51d_positive_uyr.pdf
- Song, H., Dicks, E., Ramus, S. J., Tyrer, J. P., Intermaggio, M. P., Hayward, J., ... Pharoah, P. D. (2015). Contribution of Germline Mutations in the RAD51B, RAD51C, and RAD51D Genes to Ovarian Cancer in the Population. Journal of clinical oncology : official journal of the American Society of Clinical Oncology, 33(26), 2901-7. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4554751/
- Gutiérrez‐Enríquez, S. , Bonache, S. , Ruíz de Garibay, G. , Osorio, A. , Santamariña, M. , Ramón y Cajal, T. … Diez, O. (2014). About 1% of the breast and ovarian Spanish families testing negative for BRCA1 and BRCA2 are carriers of RAD51D pathogenic variants. Int. J. Cancer, 134: 2088-2097. Retrieved from https://onlinelibrary.wiley.com/doi/full/10.1002/ijc.28540
- Mayo Clinic. Ovarian Cancer Treatment and Drugs (2018, Jan. 13). Retrieved from https://www.mayoclinic.org/diseases-conditions/ovarian-cancer/diagnosis-treatment/drc-20375946
- Reh, W. A., Nairn, R. S., Lowery, M. P., & Vasquez, K. M. (2016). The homologous recombination protein RAD51D protects the genome from large deletions. Nucleic acids research, 45(4), 1835–1847. doi:10.1093/nar/gkw1204
- Malwina, S., Katarzyna, K., Jasinska, A., Piotr, K. (2019, in press). Large-scale meta-analysis of mutations identified in panels of breast/ovarian cancer-related genes — Providing evidence of cancer predisposition genes. Gynecologic Oncology. doi: 10.1016/j.ygyno.2019.01.027
- Kurian, A., Hughes, E., Handorf, E. A., Gutin, A., Allen, B., Hartman, R., Hall, M. J. (2017). Breast and Ovarian Cancer Penetrance Estimates Derived From Germline Multiple-Gene Sequencing Results in Women. JCO Precision Oncology, [1], 1-12. doi: 10.1200/PO.16.00066
References - Images:
Background Image: https://tat.gu.se/digitalAssets/1331/1331718_tum--r.jpg
|
|